Senaman kawalan motor untuk sakit belakang bahagian bawah akut yang tidak spesifik
Referencias
References to studies included in this review
References to studies excluded from this review
Additional references
Characteristics of studies
Characteristics of included studies [ordered by study ID]
Ir a:
| Methods | Randomised controlled trial | |
| Participants | 33 participants were recruited between July 2008 and June 2010 from within a primary care musculoskeletal physiotherapy service in the London borough of Hillingdon Participants were excluded if they demonstrated evidence of any of the following: degenerative conditions affecting the spine, diabetes, pregnancy, underlying neurological conditions, active treatment of an ongoing spinal condition, active legal/compensation procedures, a history of depression, a history of multiple recurrent episodes of LBP and involvement in other research studies. Participants for whom English was not their primary language were also excluded | |
| Interventions | All patients referred for treatment of non‐specific low back pain within physiotherapy service providers were assessed and subsequently offered a place in a “core stability” class consisting of both specific and global trunk exercises. Participants in both groups received this protocol as minimum intervention. The intervention group received further instruction on 8 specific exercises for stabilisation of muscles involving the transversus abdominis (TrA) and the lumbar multifidus (LM) Core stability exercises (CSEs): Selection of exercises used in this study therefore relied on current belief systems, suggesting that isolation of TrA and LM is important for trunk stability. These exercises included the following: abdominal hollowing in prone lying, alternate straight‐leg raise in supine, abdominal hollowing in sitting, Crook lying–alternate heel slide, 4‐point kneeling pelvic shift (side to side), trunk curl in crook lying, pelvic tilt in sitting and alternate knee raise in sitting. Exercises met suggested criteria for safety, including avoidance of active hip flexion with fixed positioning of feet and pulling with the hands behind the head, while ensuring knee and hip flexion during all upper body exercises. Intervention group participants were required to perform 10 repetitions of each of the above exercises 3 times a day. To facilitate compliance, participants were required to complete a compliance diary. The diary method was chosen to avoid adding to participants' perceived barriers to exercise by impinging on available time to do the exercise routine | |
| Outcomes | Pain: assessed by a VAS comprising a 100‐mm line with no numbers Disability: assessed by the Roland Morris Disability Questionnaire Both outcomes were measured at the start of the study and at 3, 6 and 12 weeks subsequently | |
| Notes | No funding sources or conflicts of interest were reported for this study | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | "The randomization was done by a colleague independent and blind to the study using concealed envelopes within which the group description was randomly placed within them. The envelopes were numbered sequentially and chosen by the participants in the order in which they were recruited" |
| Allocation concealment (selection bias) | Low risk | "The randomization was done by a colleague independent and blind to the study using concealed envelopes within which the group description was randomly placed within them. The envelopes were numbered sequentially and chosen by the participants in the order in which they were recruited" |
| Blinding of participants and personnel (performance bias) | Low risk | "Although the participants were randomly allocated as they were recruited and blinded to the study, it was not possible to blind the assessment process" |
| Blinding of personnal/care provider (performance bias) | High risk | Care provider was not blinded |
| Blinding of outcome assessment (detection bias) | High risk | "Data were collected by the researcher who was therefore not blinded to the grouping of any of the participants" |
| Incomplete outcome data (attrition bias) | Unclear risk | Not described |
| Intention‐to‐treat analysis | High risk | Not considered. "An intention‐to‐treat analysis was used with missing data replaced with the Last Observation Carried Forward for incomplete data sets". |
| Selective reporting (reporting bias) | Low risk | Published report clearly included all expected outcomes |
| Group similarity of baseline (selection bias) | Low risk | Participants did not differ in baseline characteristics, as shown in Table 2 |
| Co‐interventions (performance bias) | Unclear risk | Not described |
| Compliance (performance bias) | Unclear risk | Not described |
| Timing of outcome assessment (detection bias) | Low risk | All important outcomes assessments for both groups were measured at the same time |
| Methods | Randomised controlled trial | |
| Participants | 123 participants. Primary recruitment occurred at a single clinic between January 1, 2000, and July 1, 2003. Additional recruitment occurred at 2 other clinics between January 1, 2002, and September 1, 2002. Each clinic was located in Utah and was affiliated with Intermountain Health Care System Inclusion criteria: Patients between 18 and 65 years of age with a primary complaint of LBP of less than 90 days' duration, with or without referral into the lower extremity, and an Oswestry Disability score of 25% were eligible Exclusion criteria: visible lateral shift or acute kyphotic deformity, signs of nerve root compression (positive straight‐leg raise test and reflex or strength deficits), any red flags indicating serious pathology such as spinal neoplasm, infection or fracture, inability to reproduce any symptoms with lumbar spine active range of motion (AROM) or palpation, current pregnancy, prior surgery to the lumbar and/or sacral region | |
| Interventions | All participants were scheduled for treatment twice weekly for 4 weeks for a maximum of 8 sessions Manipulation treatment group: Participants randomly assigned to the manipulation group were treated via manual therapy techniques, which could include thrust manipulation, or by low‐amplitude mobilisation procedures directed to the lumbosacral region, and were given instruction on a lumbar active range of motion exercise. The therapist providing treatment was permitted to reexamine the participant and could choose 1 of 2 manual therapy techniques. The decision on which technique to use was left to the therapist's discretion, but 1 of the 2 techniques had to be used. With the first technique, the participant was supine, with the lumbar spine placed into side‐bending and rotation to the opposite direction. The therapist delivered a force through the participant's pelvis in a posterior and inferior direction. For the second technique, the participant was side‐lying. The lumbar spine was positioned in flexion or extension followed by rotation in an attempt to isolate forces to a particular spinal level. The therapist delivered the force through the participant's pelvis and trunk. Selection of technique was left to the discretion of the therapist. AROM exercise was performed by instructing the participant to alternately flex and extend the lumbar spine while in a quadruped position. Specific exercise treatment group: Participants in the specific exercise group received instruction on repeated range of motion (ROM) exercises into lumbar flexion or extension. All participants in this group had to be treated using directional exercises; however, the direction of the exercise was determined by the treating therapist on the basis of reassessment of the participant's response to movement testing and symptom response to the position of sitting, standing or walking. Flexion exercises were used for participants who centralised with or had a preference for flexion movements or positions (i.e. sitting), whereas extension exercises were used for participants who centralised or had a preference for extension (i.e. standing or walking). Flexion or extension exercises were used, but not both. Flexion exercises were performed with the participant sitting, supine or quadruped. Extension exercises were performed in prone, while using prone on elbows or prone press‐up activities Stabilisation treatment group: Participants in the stabilisation group were treated with a programme of trunk strengthening and stabilisation exercises. Participants were instructed to perform abdominal bracing exercises in supine and quadruped positions, progressing to more functional positions and activities as described by Richardson and Jull. Participants were also instructed on alternating arm and leg extension exercises in quadruped to strengthen the lumbar extensor muscles. Strengthening for the oblique abdominals included curl‐up and side support exercises | |
| Outcomes | Pain: 11‐point rating scale (0 no pain to 10 worst imaginable pain) to assess current pain intensity Disability: Modified Oswestry Questionnaire (OSW) to assess disability related to LBP | |
| Notes | Supported by a research grant from the Deseret Foundation. Foundation funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the topic of this study | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | "A random number generator was used to generate a randomization list before initiation of the study. The list was maintained by the secretarial staff of the participating clinics" |
| Allocation concealment (selection bias) | Unclear risk | Sequence generation procedure or method of allocation was not mentioned |
| Blinding of participants and personnel (performance bias) | High risk | No mention of any attempts to blind participants |
| Blinding of personnal/care provider (performance bias) | High risk | No mention of any attempts to blind care provider |
| Blinding of outcome assessment (detection bias) | High risk | "Baseline and follow‐up examinations were conducted by a physical therapist who remained blind to the treatment group assignment"; outcome measures were self reported, thus, assessor was not considered blinded |
| Incomplete outcome data (attrition bias) | High risk | "Eighty one patients (66%) completed the long‐term follow‐up, with no differences in the median number of days between baseline and follow‐up or the proportions of patients with completed follow‐up between patients receiving matched or unmatched treatments" |
| Intention‐to‐treat analysis | Low risk | "Analysis was performed using intention‐to‐treat principles, with the last available OSW score carried forward for any missing data" |
| Selective reporting (reporting bias) | Low risk | Published report clearly included all expected outcomes |
| Group similarity of baseline (selection bias) | Low risk | Participants did not differ in baseline characteristics, as presented in Table 1, and no differences were found in additional data provided by study authors |
| Co‐interventions (performance bias) | Unclear risk | Not described |
| Compliance (performance bias) | Low risk | Compliance was acceptable on the basis of reported intensity/dosage, duration, number and frequency for all 3 groups |
| Timing of outcome assessment (detection bias) | Low risk | All important outcomes assessments for both groups were measured at the same time |
| Methods | Randomised controlled trial | |
| Participants | 41 patients recruited from an accident and emergency department at a hospital over a 6‐month period Inclusion criteria: Men and women were eligible for the study in the first instance if they were 18 to 45 years of age and were experiencing their first episode of unilateral, mechanical LBP for less than 3 weeks Exclusion criteria: previous history of LBP or injury, previous lumbar surgery, spinal abnormalities indicated on radiographs, neuromuscular or joint disease, reflex and/or motor signs of nerve root compression or cauda equina compression, evidence of systemic disease, carcinoma or organ disease, pregnancy, any sports or fitness training involving the low back muscles done in the past 3 months | |
| Interventions | Medical management group: advice on bed rest and absence from work and prescription of medication. Minimal bed rest (1 to 3 days) and only minor analgesics were prescribed. These analgesics included aspirin, paracetamol, combinations of low doses of codeine and aspirin, non‐steroidal anti‐inflammatory agents, Digestics and Capadex. Prescription of Valium was also allowable Exercise therapy: Therapeutic exercises were designed to re‐educate the multifidus muscle in its stabilising role. They involved facilitating an active, isometric multifidus contraction in co‐contraction with deep abdominal muscles. Participants performed the contraction in the standing position with the lumbar spine in a neutral position. Contraction of the multifidus was confirmed by real‐time ultrasound imaging | |
| Outcomes | Pain: McGill Pain Questionnaire and visual analogue scales Disability: Roland Morris Disability Index | |
| Notes | Financial support from The Menzies Foundation, The JP Kelly Mater Research Foundation, The Wenkart Foundation, The Physiotherapy Research Foundation and the Manual Therapy Special Group (Australia) | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | "Random assignment to the control or treatment group was achieved by selecting the group number from sealed, shuffled envelopes" |
| Allocation concealment (selection bias) | Low risk | "Random assignment to the control or treatment group was achieved by selecting the group number from sealed, shuffled envelopes" |
| Blinding of participants and personnel (performance bias) | High risk | No mention of any attempts to blind participants |
| Blinding of personnal/care provider (performance bias) | High risk | No mention of any attempts to blind care provider |
| Blinding of outcome assessment (detection bias) | High risk | "Assessments were performed by two independent examiners, who were blinded to group allocation and patient presentation"; outcome measures were self reported, thus, assessor was not considered blinded |
| Incomplete outcome data (attrition bias) | Low risk | Percentages of withdrawals and dropouts were within the acceptable rate |
| Intention‐to‐treat analysis | Unclear risk | Not described |
| Selective reporting (reporting bias) | Low risk | Published report clearly included all expected outcomes |
| Group similarity of baseline (selection bias) | High risk | Groups were not similar at baseline regarding outcome disability |
| Co‐interventions (performance bias) | Unclear risk | Not described |
| Compliance (performance bias) | Unclear risk | Not described |
| Timing of outcome assessment (detection bias) | Low risk | All important outcomes assessments for both groups were measured at the same time |
AROM: active range of motion.
CSE: core stability exercise.
LBP: low back pain.
LM: lumbar multifidus.
OSW: Modified Oswestry Questionnaire.
ROM: range of motion.
TrA: transversus abdominis
Characteristics of excluded studies [ordered by study ID]
Ir a:
| Study | Reason for exclusion |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| No patients with non‐specific LBP | |
| All groups given MCE | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Chronic LBP | |
| Not an RCT | |
| Chronic LBP | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No patients with non‐specific LBP | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No patients with non‐specific LBP | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| Not an RCT | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No evaluation of relevant outcomes for this review | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No patients with non‐specific LBP | |
| Chronic LBP | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| No evaluation of relevant outcomes for this review | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| All groups given MCE | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| Protocol | |
| Not an RCT | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| All groups given MCE | |
| Not an RCT | |
| Not an RCT | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| All groups given MCE | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Not an RCT | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No patients with non‐specific LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| Chronic LBP | |
| Not an RCT | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| No patients with non‐specific LBP | |
| No MCE and no mixed intervention | |
| All groups given MCE | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| Chronic LBP | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| Not an RCT | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention | |
| No MCE and no mixed intervention |
LBP: low back pain.
MCE: motor control exercise.
RCT: randomised controlled trial.
Data and analyses
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 1.1  Comparison 1 Motor control exercise vs spinal manipulative therapy, Outcome 1 Pain. | ||||
| 1.1 Short term | 1 | 58 | Mean Difference (IV, Random, 95% CI) | 9.0 [‐1.56, 19.56] |
| 2 Disability Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 1.2 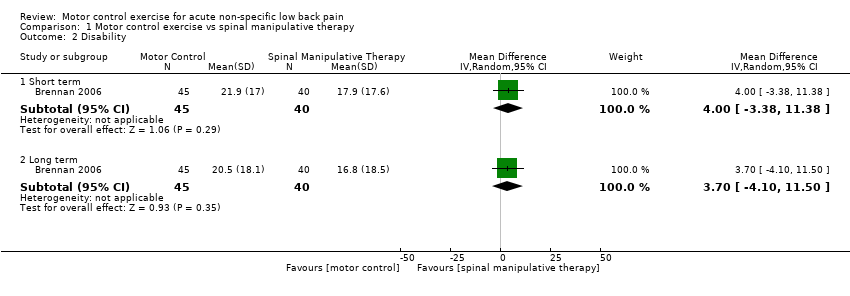 Comparison 1 Motor control exercise vs spinal manipulative therapy, Outcome 2 Disability. | ||||
| 2.1 Short term | 1 | 85 | Mean Difference (IV, Random, 95% CI) | 4.0 [‐3.38, 11.38] |
| 2.2 Long term | 1 | 85 | Mean Difference (IV, Random, 95% CI) | 3.70 [‐4.10, 11.50] |
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 2 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 2.1  Comparison 2 Motor control exercise vs other exercises, Outcome 1 Pain. | ||||
| 1.1 Short term | 2 | 89 | Mean Difference (IV, Random, 95% CI) | 5.74 [‐3.34, 14.82] |
| 1.2 Intermediate term | 1 | 33 | Mean Difference (IV, Random, 95% CI) | ‐1.20 [‐18.24, 15.84] |
| 2 Disability Show forest plot | 2 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 2.2  Comparison 2 Motor control exercise vs other exercises, Outcome 2 Disability. | ||||
| 2.1 Short term | 2 | 116 | Mean Difference (IV, Random, 95% CI) | ‐0.84 [‐8.72, 7.04] |
| 2.2 Intermediate term | 1 | 33 | Mean Difference (IV, Random, 95% CI) | ‐6.70 [‐22.80, 9.40] |
| 2.3 Long term | 1 | 83 | Mean Difference (IV, Random, 95% CI) | 5.70 [‐1.38, 12.78] |
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 3.1  Comparison 3 Motor control exercise as a supplement to medical management, Outcome 1 Pain. | ||||
| 1.1 Short term | 1 | 41 | Mean Difference (IV, Random, 95% CI) | ‐9.3 [‐20.41, 1.81] |
| 2 Disability Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| Analysis 3.2 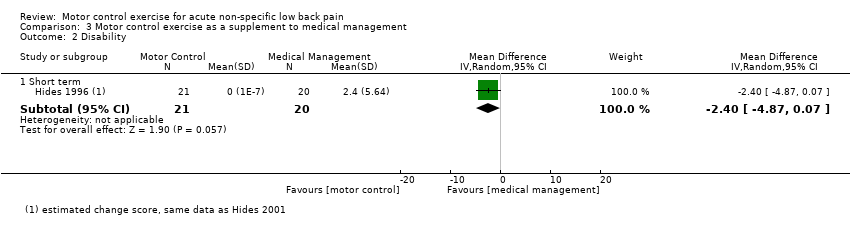 Comparison 3 Motor control exercise as a supplement to medical management, Outcome 2 Disability. | ||||
| 2.1 Short term | 1 | 41 | Mean Difference (IV, Random, 95% CI) | ‐2.4 [‐4.87, 0.07] |
| 3 Recurrence Show forest plot | 1 | Risk Ratio (M‐H, Random, 95% CI) | Subtotals only | |
| Analysis 3.3  Comparison 3 Motor control exercise as a supplement to medical management, Outcome 3 Recurrence. | ||||
| 3.1 Long term | 1 | 39 | Risk Ratio (M‐H, Random, 95% CI) | 0.36 [0.18, 0.72] |
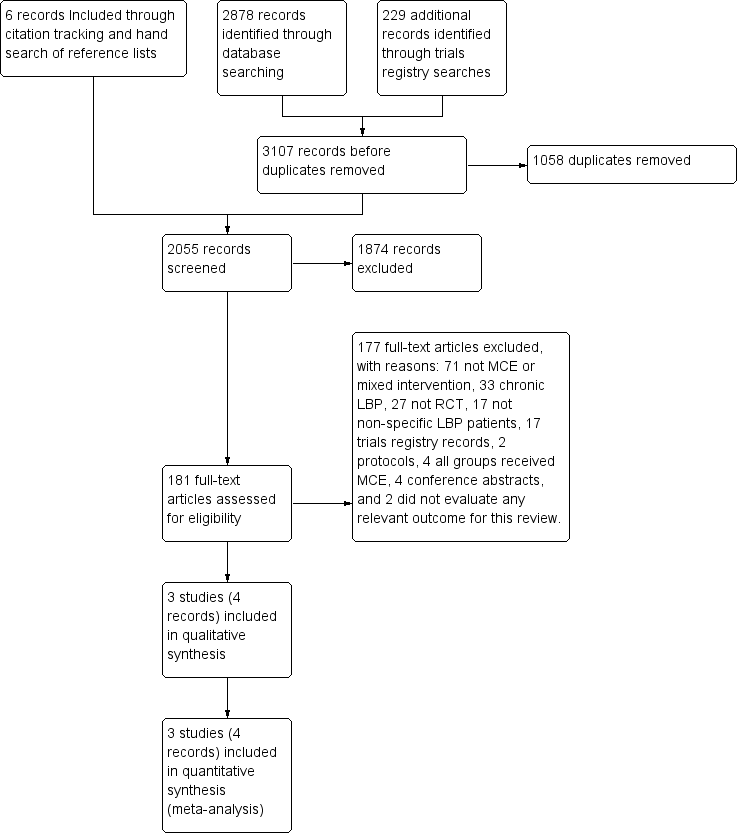
Study flow diagram.

Risk of bias summary: review authors' judgements about each risk of bias item for each included study.

Forest plot of comparison: 2 Motor control exercise vs other exercises, outcome: 2.1 Pain.
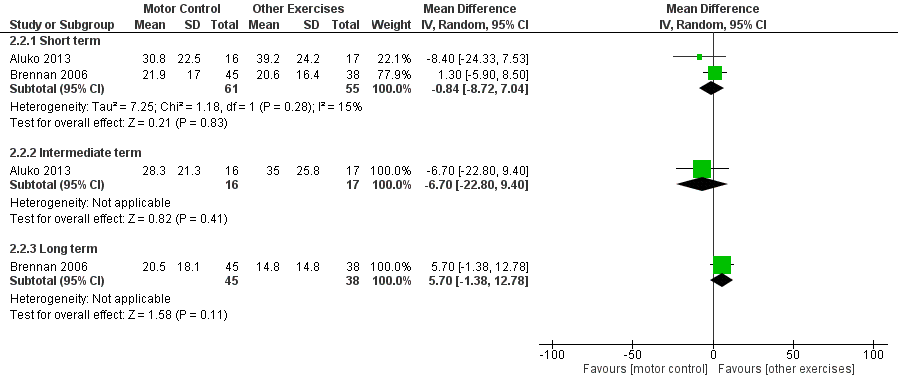
Forest plot of comparison: 2 Motor control exercise vs other exercises, outcome: 2.2 Disability.

Comparison 1 Motor control exercise vs spinal manipulative therapy, Outcome 1 Pain.
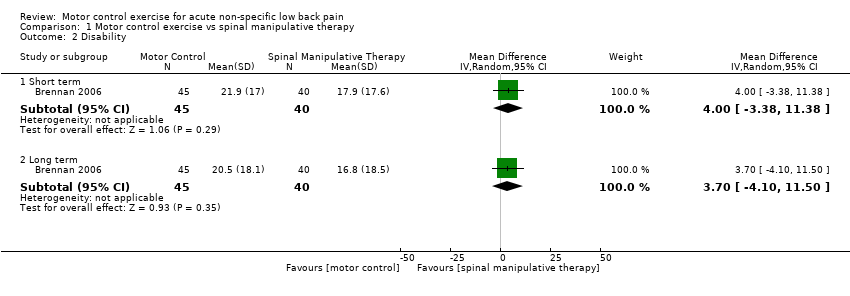
Comparison 1 Motor control exercise vs spinal manipulative therapy, Outcome 2 Disability.

Comparison 2 Motor control exercise vs other exercises, Outcome 1 Pain.
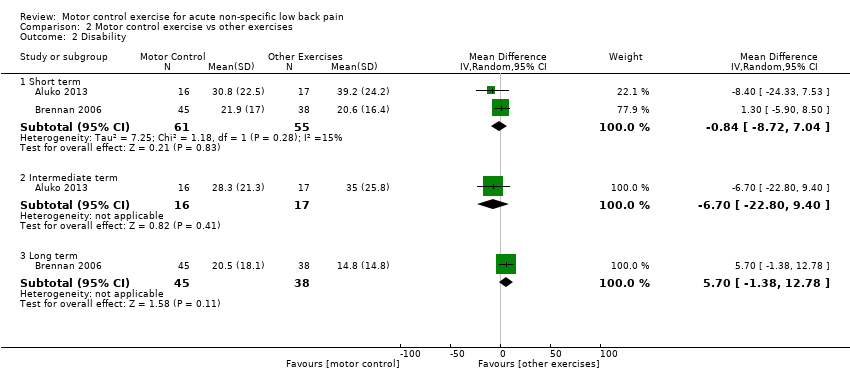
Comparison 2 Motor control exercise vs other exercises, Outcome 2 Disability.
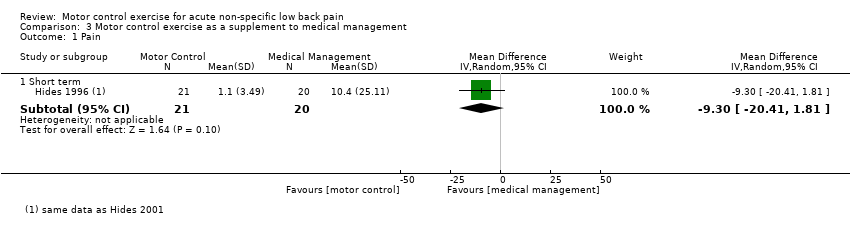
Comparison 3 Motor control exercise as a supplement to medical management, Outcome 1 Pain.
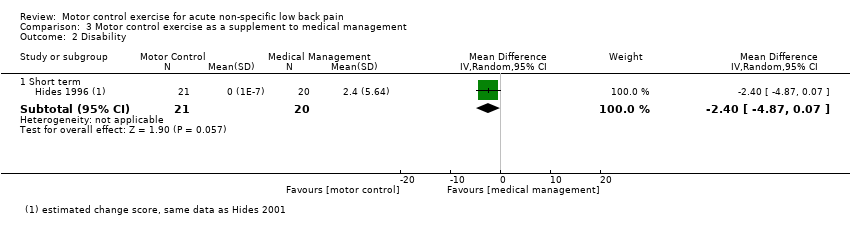
Comparison 3 Motor control exercise as a supplement to medical management, Outcome 2 Disability.

Comparison 3 Motor control exercise as a supplement to medical management, Outcome 3 Recurrence.
| Motor control exercise vs spinal manipulative therapy for acute low back pain | ||||
| Patient or population: patients with acute low back pain Settings: primary or tertiary care Intervention: motor control exercise Comparison: spinal manipulative therapy | ||||
| Outcomes | Illustrative comparative risks* (95% CI) | Number of participants | Quality of the evidence | |
| Assumed risk | Corresponding risk | |||
| Spinal manipulative therapy | Motor control exercise | |||
| Pain VAS (0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean pain in the control group was 15 points | Mean pain in the intervention group was 9 points higher (1.56 lower to 19.56 higher) | 58 participants (1 study) | ⊕⊕⊝⊝ |
| Disability Oswestry Disability Index (0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean disability in the control group was 17.9 points | Mean disability in the intervention group was 4 points higher (3.38 lower to 11.38 higher) | 85 participants | ⊕⊕⊝⊝ |
| Disability Oswestry Disability Index (0 to 100) Follow‐up: intermediate term (> 3 months, < 12 months) | Mean disability in the control group was 16.8 points | Mean disability in the intervention group was 3.7 points higher (4.10 lower to 11.50 higher) | 85 participants | ⊕⊕⊝⊝ |
| Adverse events None of the included studies evaluated adverse events | Not reported | Not reported | ||
| *The basis for the assumed risk (e.g. median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI) | ||||
| GRADE Working Group grades of evidence | ||||
| aDowngraded for imprecision bDowngraded for inconsistency | ||||
| Motor control exercise vs other exercises for acute low back pain | ||||
| Patient or population: patients with acute low back pain Settings: primary or tertiary care Intervention: motor control exercise Comparison: other exercises | ||||
| Outcomes | Illustrative comparative risks* (95% CI) | Number of participants | Quality of the evidence | |
| Assumed risk | Corresponding risk | |||
| Other exercises | Motor control exercise | |||
| Pain VAS (0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean pain ranged across control groups from | Mean pain in the intervention groups was 5.74 points higher (3.34 lower to 14.82 higher) | 89 participants | ⊕⊕⊕⊝ |
| Pain VAS (0 to 100) Follow‐up: intermediate term (> 3 months, < 12 months) | Mean pain in the control group was | Mean pain in the intervention groups was 1.2 points lower (18.24 lower to 15.84 higher) | 33 participants | ⊕⊕⊝⊝ |
| Disability Multiple scales (transformed 0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean disability ranged across control groups from | Mean disability in the intervention groups was 0.84 points lower (8.72 lower to 7.04 higher) | 116 participants | ⊕⊕⊕⊝ |
| Disability Roland Morris Disability Questionnaire (transformed 0 to 100) Follow‐up: intermediate term (> 3 months, < 12 months) | Mean disability in the control group was | Mean disability in the intervention groups was 6.70 points lower (22.80 lower to 9.40 higher) | 33 participants | ⊕⊕⊝⊝ |
| Disability Oswestry Disability Index (0 to 100) Follow‐up: long term (< 3 months after randomisation) | Mean disability in the control group was 20.5 | Mean disability in the intervention groups was (1.38 lower to 12.78 higher] | 83 participants | ⊕⊕⊝⊝ |
| Adverse events None of the included studies evaluated adverse events | Not reported | not reported | ||
| *The basis for the assumed risk (e.g. median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI) | ||||
| GRADE Working Group grades of evidence | ||||
| aDowngraded for imprecision bDowngraded for inconsistency | ||||
| Motor control exercise as a supplement to medical management for patients with acute low back pain | |||||
| Patient or population: patients with acute LBP Settings: primary or tertiary care Intervention: motor control exercise Comparison: medical management | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | Relative effect | Number of participants | Quality of the evidence | |
| Assumed risk | Corresponding risk | ||||
| Medical management | Motor control exercise | ||||
| Pain VAS (0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean pain in the control group was | Mean pain in the intervention group was 9.30 points lower (20.41 lower to 1.81 higher) | 41 participants | ⊕⊕⊝⊝ | |
| Disability Roland Morris Disability Questionnaire (transformed 0 to 100) Follow‐up: short term (< 3 months from randomisation) | Mean disability in the control group was 2.4 | Mean disability in the intervention group was (4.87 lower to 0.07 higher) | 41 participants | ⊕⊕⊝⊝ | |
| Recurrence Follow‐up: long term (1 year) | 16 of 19 | 6 of 20 | RR 0.36 (0.18 to 0.72) | 39 participants (1 study) | ⊕⊕⊝⊝ |
| Adverse events None of the included studies evaluated adverse events | Not reported | Not reported | |||
| *The basis for the assumed risk (e.g. median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI) | |||||
| GRADE Working Group grades of evidence | |||||
| aDowngraded for imprecision bDowngraded for inconsistency cDowngraded for high risk of bias | |||||
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 1.1 Short term | 1 | 58 | Mean Difference (IV, Random, 95% CI) | 9.0 [‐1.56, 19.56] |
| 2 Disability Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 2.1 Short term | 1 | 85 | Mean Difference (IV, Random, 95% CI) | 4.0 [‐3.38, 11.38] |
| 2.2 Long term | 1 | 85 | Mean Difference (IV, Random, 95% CI) | 3.70 [‐4.10, 11.50] |
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 2 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 1.1 Short term | 2 | 89 | Mean Difference (IV, Random, 95% CI) | 5.74 [‐3.34, 14.82] |
| 1.2 Intermediate term | 1 | 33 | Mean Difference (IV, Random, 95% CI) | ‐1.20 [‐18.24, 15.84] |
| 2 Disability Show forest plot | 2 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 2.1 Short term | 2 | 116 | Mean Difference (IV, Random, 95% CI) | ‐0.84 [‐8.72, 7.04] |
| 2.2 Intermediate term | 1 | 33 | Mean Difference (IV, Random, 95% CI) | ‐6.70 [‐22.80, 9.40] |
| 2.3 Long term | 1 | 83 | Mean Difference (IV, Random, 95% CI) | 5.70 [‐1.38, 12.78] |
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
| 1 Pain Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 1.1 Short term | 1 | 41 | Mean Difference (IV, Random, 95% CI) | ‐9.3 [‐20.41, 1.81] |
| 2 Disability Show forest plot | 1 | Mean Difference (IV, Random, 95% CI) | Subtotals only | |
| 2.1 Short term | 1 | 41 | Mean Difference (IV, Random, 95% CI) | ‐2.4 [‐4.87, 0.07] |
| 3 Recurrence Show forest plot | 1 | Risk Ratio (M‐H, Random, 95% CI) | Subtotals only | |
| 3.1 Long term | 1 | 39 | Risk Ratio (M‐H, Random, 95% CI) | 0.36 [0.18, 0.72] |

